Perhaps lost in the shuffle last year due to the implementation of ICD-10, was the creation of MACRA, which was signed into legislation by President Obama on April 16, 2015. Fast forward one year later to current day and the recently proposed MACRA rules, which have been described as the most significant Medicare policy change in recent history.
What is it?
MACRA replaces the sustainable growth rate (SGR) formula with a framework that rewards providers for providing higher quality care through the creation of two reimbursement pathways:
- Merit-based incentive Payment System (MIPS), and
- Alternative Payment Models (APMs).
Additionally, the proposed rules collapse three existing quality reporting programs (PQRS, Value-based Payment Modifier, and Meaningful Use) into the newly created MIPS pathway. Not all providers will receive positive reimbursement adjustments. In fact, CMS estimates that 45% of eligible providers and up to 87% of small group practices will see a penalty in the first payment year.
Most physicians that bill Medicare Part B claims will be impacted. Rural health clinics and FQHC providers are excluded.
When do changes occur?
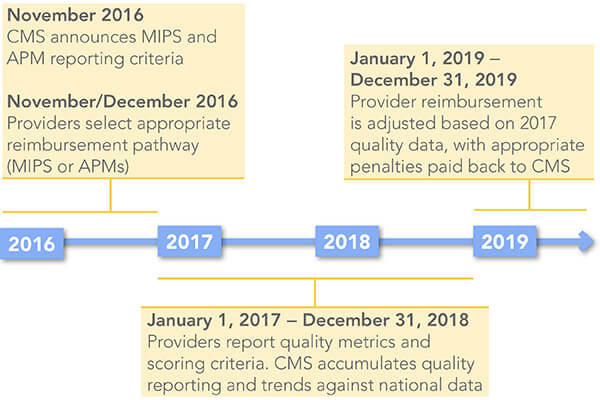
Note: In less than five months, providers will select the quality metrics that will impact their 2019 Medicare reimbursement.
Significance
Starting in 2019, Medicare provider reimbursement will be impacted either positively or negatively based on 2017 quality data. Since CMS projects that the majority of providers will follow the MIPS track, the following outlines the proposed Medicare Part B reimbursement impact under that pathway:
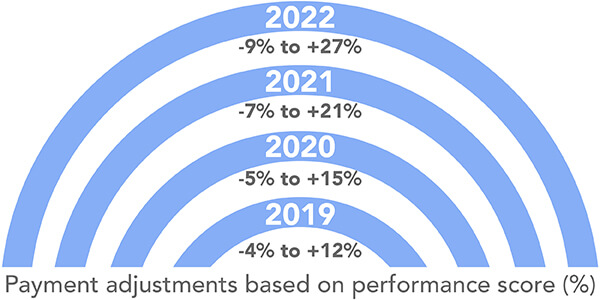
MACRA ensures that there will only be increases or decreases in Medicare Part B reimbursement – it is budget neutral in aggregate. To ensure your Medicare Part B reimbursement is protected against these future penalties, now is the time to assess your readiness and implement operational changes that might be needed to potentially share in the reimbursement increases scheduled in 2019.
Contact Adam Shewmaker at ashewmaker@ddafhealthcare.com or Porter Roberts at proberts@deandorton.com to learn more.
